When we consider our 2-3 million year evolution it stands to reason that our bodies are best adapted to the hunter-gatherer diet of our Paleolithic ancestors. Although the assumption is often made that agriculture was in every respect an improvement upon the human condition, anthropological research shows that if our Paleolithic ancestors were able to survive accidents, infection and childbirth, their longevity was similar to that of the modern human, but without many of the chronic degenerative diseases that affect us now. These conclusions are bolstered by contemporary research on the last few remaining Paleolithic groups such as the !Kung peoples of the Kalahari and Aché peoples of Paraguay, who are remarkably free of the chronic degenerative diseases that plague the industrialized world. The accounts of the first European explorers in North America are replete with references to the robust health and vitality of the Native Americans, who displayed little indication of the disease and pestilence the explorers left behind across the Atlantic. In the few hundred years since colonization and the adoption of the European diet, however, Native Americans now suffer from the highest rates of diabetes, cardiovascular disease and cancer in North America. From “robust” health to chronically infirm in just a few centuries, the Native American experience is only the most recent tale in the 10,000 years saga of our collective experiment with agriculture.
Cultivating a Paleolithic diet
The hallmark of the Paleolithic diet is an avoidance of agricultural staples including cereal grains, legumes, some types of nuts and seeds, dairy, refined vegetable oils and sweeteners. Although this apparently limits the diversity of the diet, many people are remarkably unaware of just how few types of foods we eat nowadays. Take a look in the shopping cart of your average shopper at the grocery store, and you will likely find the same five products such as milk, potatoes, wheat, corn and sugar. So while avoiding such foods may seem initially restrictive, it does out of necessity open up entirely new vistas in food previously unimagined.
- Protein-based foods on the Paleolithic diet include all pasture-raised, forage-fed or wild animal products, including meat, eggs, poultry, and fish (p. 53). Plant sources for proteins include nuts and seeds (p. 68) but as these contain allergens and anti-nutrient factors people with sensitive immune systems should approach them with caution.
- Fat-based foods include all fats naturally found in animal products, as well as the fat rendered from them including tallow, grease and lard (p. 233), and fatty vegetable foods such as coconut and avocado. Clarified butter (ghee) (p. 231) is not a Paleolithic food, but as it is rendered from sugars and immunoreactive proteins it is an acceptable food that rarely provokes a negative response.
- Carbohydrate-based foods include glycogen-rich animal tissues such as liver, as well as wild roots and tubers, wild fruits, and inner tree bark. In the Paleolithic diet I also include most root vegetables such as beets, rutabaga and Jerusalem artichoke as well as winter squashes and non-gluten grains such as quinoa, amaranth, rice and buckwheat (p. 57), although very sensitive individuals may need to avoid cereals and legumes entirely (see Food sensitivities and allergies, p. 271). All non-starchy vegetables (p. 43) are acceptable in the Paleolithic diet with the possible exception of nightshades, including tomato, eggplant and bell peppers, which can provoke inflammation in sensitive individuals (p. 271).
- Restricted foods include cereal grains (p. 57), legumes (p. 64), dairy (p. 71), sweet fruits (p. 49), sweeteners (p. 89), coffee and chocolate (p.93), alcohol (p. 99), and for insulin resistance and diabetes, very starchy vegetables such as sweet potato, yam, potato, cassava, taro, dasheen and tapioca (p. 43). Sometimes not all these foods need be eliminated permanently, and can simply be consumed in smaller amounts.
The dietary ratio of proteins, carbohydrates and fats among Paleolithic peoples varied considerably depending on culture and geography, anywhere from 19–35% for proteins, 22–40% for carbohydrates, and 28–58% for fats. One major factor missing from this equation, however, is the abundance of low-calorie non-starchy vegetation such as leafy greens, which are otherwise rich in trace minerals, vitamins and accessory nutrients. In my practice I suggest that when possible these foods comprise upwards of 50% of the total volume of foods eaten each to help to promote good digestion and moderate the appetite (see page 43, Food As Medicine).
While the Paleolithic diet may seem restrictive when compared to the typical Western diet, many people find that the immediate health benefits out-weigh the inconvenience. It is a diet that has low immunogenicity or allergy-causing potential, and thus people with food sensitivities and allergies often experience a lessening of symptoms when they have been on this diet for as little as a 1-2 weeks. Even environmental allergies such as animal dander or pollen lessen to the point of tolerance, and sometimes cease all together.
With appropriate support this kind of diet can be very helpful in modulating the activity of autoimmune disorders such as multiple sclerosis and rheumatoid arthritis. In the treatment of chronic digestive disorders such as irritable bowel syndrome and Crohn’s disease, the Paleolithic diet can be very helpful to lessen the reactivity of the gastric mucosa and normalize digestion. With its absence of refined carbohydrates the Paleolithic diet effectively inhibits fungal growth and development, and is useful to control chronic candidiasis (yeast) and related chronic fungal infections (e.g. fungal rhinosinusitis). In the same way, the Paleolithic diet helps to normalize blood sugar and insulin levels, which in turn reduces the risk of diseases associated with insulin resistance including truncal obesity, hypertension, cardiovascular disease and diabetes.
Although it is no miracle, the changes many people experience on this diet do indeed seem miraculous. In my clinical experience, however, some symptoms can actually worsen during the first few weeks of treatment, only to resolve some four to six weeks later. In traditional medicine this is described as a “healing crisis”: when the immune response shifts from a state of relative tolerance to an aggressive response that redirects the body back to homeostatic balance. At around the sixth week mark approximately half the blood cells in the body have been replaced, and thus it is only after this time that the effect of the dietary change overcomes the inertia of the inflammatory response.
Since the first publication of this book, the Paleolithic diet has moved into the mainstream, and with it’s increasing popularity, a number of vocal critics that have taken issue with it. Most of the arguments revolve around what critics perceive to be an overly simplistic understanding of what exactly our Paleolithic ancestors ate. As the Paleolithic diet has things in common with the Atkins diet, some people think that they are entirely interchangeable. But the emphasis upon animal fats and proteins, and a reduction in plant-based foods found in some versions of the Atkins diet, is not reflective of Paleolithic nutrition. The first thing to realize is that apart from the absence of agricultural staples, the Paleolithic diet was enormously varied, depending on geography, climate, culture, and local resources. In tropical climates with year-round growing conditions, the Paleolithic diet was rich in vegetation, whereas the diet of Paleolithic peoples living in sub-arctic conditions was comprised mostly of animal fat and protein. Thus there was never “one” type of Paleolithic diet: it still must be adapted to individual needs and circumstances. As safe bet, however, I recommend to my patients that at least 50% of the volume of food they eat every day be above-ground vegetables. The remainder of the diet should be an individual-specific balance of starches, fats and proteins (see p. 30, Food As Medicine). One thing is clear: ancient peoples relied upon a great diversity of plant species as food and medicine: and oftentimes, they were the same thing. Prepared according to the doshas (p. 47, Food As Medicine), eating a varied, mostly plant-based diet is the best protection against chronic disease.
Paleolithic diet ratios
Taking all of the information from above, let’s look at how much of each category of food you should try to emphasize in your diet. The following dietary ratios are based not on caloric intake, but rather, a rough estimate of the volume of each food group you eat on a daily basis. In other words, imagine all these foods sitting on a plate at a meal, and the comparative volumes they comprise while sitting on the plate. For a variety of reasons, including the fact that the scientific methods used to determine the caloric content of different foods doesn’t equate with real-time metabolic processes, we shall discard the concern over calories for now. Anyway, most people don’t eat this way: they eat with their senses, not with a calorimeter or the rigorous application of calorie tables. Generally speaking, eat until your hunger is satisfied, but not until you are “stuffed.” In Ayurvedic medicine we are told to eat to “one-half” our stomach volume at each meal, moistened with 1/4 part water, leaving 1/4 part of your stomach to accommodate gastric churning.
- Animal products: 20-30 %
- Non-starchy vegetables (above ground): 40-50 %
- Starchy vegetables (roots, tubers, squash): 20-30 %
- Fruits: 5-10 %
- Fats and Oils: 5-10 %
For autoimmune diseases such as rheumatoid arthritis, inflammatory bowel disease and multiple sclerosis, foods such as grains, cereals, legumes and dairy should be strictly avoided, but otherwise, carbohydrate-rich foods such as root vegetables and seasonal fruit can be consumed in moderation without harm.
Although the Paleolithic diet may seem restrictive when compared to the typical Western diet, many people find that the immediate health benefits out-weigh the inconvenience. Please note that it may take several weeks or months for the effects of the diet to take effect, due to a “ripple effect” of consuming immunoreactive foods prior to making dietary changes.
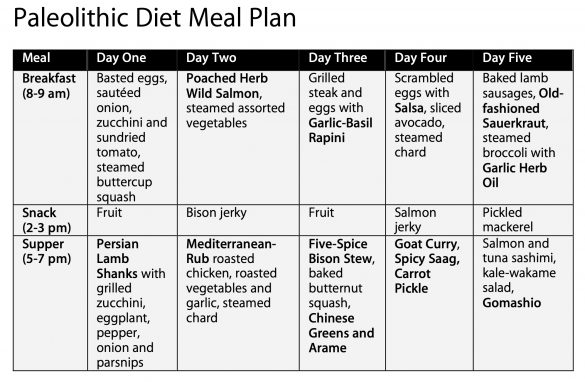
Sample meal plan
The following is a sample meal plan of the Paleolithic diet, taken from Food as Medicine. All of the recipes if represented in bold-faced type are found in the book.